Children with eczema often have to deal with days or nights of relentless itching, red patches and cracked skin. If you’re a first-time parent, you may almost helplessly watch your baby scratch and wince, wondering if there’s more you can do than slather on creams.
Here’s where a childhood eczema Specialist in Singapore comes in. Thanks to their specialised training, you can count on them to bring focused expertise in atopic dermatitis, as well as use tests and treatments beyond basic moisturisers.
You can count on them to help you pinpoint triggers, calm flare‑ups and build a long‑term care plan tailored to your child’s needs. On this page, we will show you when to seek a childhood eczema specialist for your baby and what treatments they might prescribe. But first;
What does Childhood Eczema Look Like?
Childhood eczema is also commonly known as atopic eczema. It is a common inflammatory skin condition that usually starts in early childhood and causes dry, itchy patches that tend to flare and then settle over time.
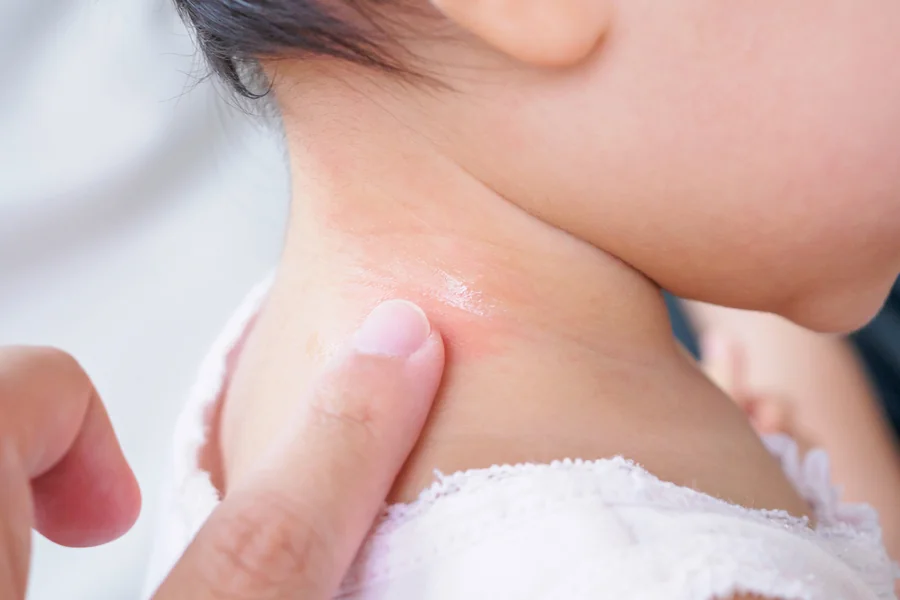
It often begins between 3 months and 5 years of age and may ease or persist into later years. You’ll see eczema as intensely itchy rash patches. In infants, this often shows as red, sometimes weepy skin on the cheeks, forehead, scalp and occasionally body, but rarely in the nappy area.
As your child grows (especially from around age 2), the rash moves into the skin folds: inside the elbows, behind the knees, neck, wrists, ankles and hands. How eczema looks depends on skin tone.
If your baby has lighter skin, the patches may appear as red or pink. If the baby has a darker skin, the patchs can be brown, grey or purple and sometimes less obviously inflamed.
Lesions may include tiny raised bumps, dry flaky areas or even blisters that ooze or crust if scratched or infected. Repeated scratching can thicken and harden affected areas in a process called lichenification.
The skin may become leathery, darker and cracked. Cracks are especially common around joints and can be painful and bleed.
When to Take a Child to the Doctor for Eczema?
If your baby has developed eczema, a mild one can easily improve with just regular moisturisers and mild over-the-counter steroid creams. Also, consistent habits like daily baths with gentle cleansers, patting skin dry, then applying moisturizer can keep flare‑ups at bay.
If your child’s rash calms after two weeks, you can continue these simple steps at home. You shouldn’t keep trying to treat your baby for eczema on your own if you notice any of these developments;
- Spreading or worsening rash: An eczema that is spreading or worsening can be characterised by a rash that once stayed on your child’s cheeks extending to arms or trunk. The skin may turn redder or thicker and feel warmer. These changes show that simple moisturisers or over‑the‑counter creams no longer help. Seek an early assessment to prevent complications and guide you towards stronger treatments.
- Severe itching affecting sleep or mood: Seek medical advice from a childhood eczema specialist if your baby experiences relentless itching that stops them from sleeping or makes them irritable. Night‑time scratching can wake them often and leave both of you tired. Lack of rest also affects concentration at school and can change your baby’s behaviour. You might see them tear at skin until it bleeds or cracks. A childhood eczema specialist can adjust treatment to reduce itching and restore comfort so they sleep and play better.
- Signs of infection: When eczema spots weep yellow fluid, ooze or form crusts, it could suggest an infection. You may see rapid redness around the rash or feel warmth on touch. Your child could also run a fever or look unwell. Infected eczema can hurt more and spread quick which is why it needs prompt treatment with antibiotics or antiviral creams. Call your childhood eczema specialist as soon as you spot these changes to avoid complications.
- Rash is painful: If your child winces or cries when you touch eczema patches, it means pain has set in. Damaged skin may crack and bleed at bend points. As you’d imagine, this can make even simple movement hard. Even gentle pressure can hurt your baby. Painful eczema needs quick assessment. The specialist can prescribe treatments to ease discomfort and repair skin. Don’t wait more than a day to call your childhood eczema specialist, especially if pain keeps your child from normal play.
- Persistence or poor response to treatment: Regular moisturisers and mild steroid creams should be able to ease your child’s eczema after about two weeks. If this doesn’t happen then surely, it is time to seek a doctor’s review. Lack of progress suggests you need a stronger prescription or different care plan. If you spot redness, dryness or itch still present after this time, don’t carry on alone. A skilled childhood eczema specialist can reassess, check for underlying issues and adjust medications to bring relief and prevent flare‑ups.
- Frequent flare‑ups or unclear diagnosis: When eczema returns too often or you’re unsure it’s truly eczema, a doctor can offer clarity. Frequent flare‑ups may point towards allergies, infections or different skin conditions. A doctor can run tests to find triggers and rule out other causes. A clear diagnosis will help you follow a better long‑term plan. A paediatric dermatologist or allergist can guide you on tailored treatments, trigger avoidance and strategies to keep your child comfortable.
What is Prescribed for Eczema in Children?
If you’re curious about what to expect at your childhood eczema specialist, a fairly common question you may also want to ask is; what is prescribed for eczema in children? Now, if your baby is diagnosed with eczema, the doctor may prescribe moisturisers (emollients) to repair the skin barrier.
These will need to be used daily, even when eczema clears. Topical corticosteroids like hydrocortisone may be prescribed for mild cases and mid to potent steroids (like triamcinolone, mometasone) for moderate to severe flare‑ups to reduce inflammation and itching.
If prescribed, these will need to be used once or twice daily for up to two weeks depending on severity and location. Your baby may also be prescribed topical calcineurin inhibitors (tacrolimus or pimecrolimus.)
These are steroid‑free options often used for sensitive areas like the face or long‑term care. PDE‑4 inhibitors like crisaborole may also be used to offer an anti‑inflammatory option with lower side‑effect risk.
If flare‑ups continue despite topicals, your childhood eczema specialist may add biologics (e.g., dupilumab) if your baby is over 6 months or phototherapy. In rare severe cases, oral immunosuppressants (like cyclosporine) can used short‑term under close supervision.
In Closing
Seeing a doctor helps keep your child comfortable and prevents complications. If you notice spread, severe itch, pain, infection, or no clear improvement, trust your instincts. Prompt medical care gives you tailored treatment guidance. That way, your child can enjoy healthier skin and better days.
Our childhood eczema specialists offer gentle care and lasting relief. Book your appointment and help your child feel truly comfortable in their skin again. Call or visit us.